The Efficacy of Ultrasound-guided Retrolaminar Block on Postoperative Analgesia for Lumbar İnstrumentation Surgery
By Kevser PekerAffiliations
doi: 10.29271/jcpsp.2020.12.1355Sir,
The retrolaminar block (RLB) is a type of paraspinal interfascial plane block that targets the vertebral lamina. The local anesthetic spreads in the paravertebral area and blocks the spinal nerve branches.1,2 Herein, we report a patient who underwent lumbar instrumentation surgery after the application of preoperative RLB for postoperative analgesia. The patient's informed consent was obtained.
A 53-year woman was scheduled for lumbar vertebra instrumentation under general anesthesia with bilateral ultrasound-guided RLBs. We performed the blockage by using a 7-18 MHz convex ultrasound probe (Esaote My Lab 6 US Machine, Florance, Italy) and a 22-gauge, 100-mm Stimuplex needle (B. Braun, Germany). We reached the sagittal plane from lateral to medial at the mid-lumbar level and identified the hyperechoic L3 laminae approximately 2 cm lateral of the spinous process (Figure 1, A-D).
 Figure 1 (A): The surface marking of the laminae.
Figure 1 (A): The surface marking of the laminae.
The needle was inserted into a plane of craniocaudal direction. After reaching the laminary contact level with negative aspiration, 20 ml bupivacaine 0.25% was injected at low pressure (Figure 1, A-D). Thirty minutes later, the patient was transferred to the operating room.
In the recovery unit and on the first postoperative day, the patient did not have an opioid requirement. The visual analogue scale (VAS) scores were four (4/10) and five (5/10) at the second and 8th hour, respectively. Dexketoprofen was used as an analgesic agent, when needed. No complications were observed, and the patient was discharged on the third postoperative day, with adequate pain control. The patient's low VAS scores and complication-free postoperative period suggested analgesic efficacy of RLB.
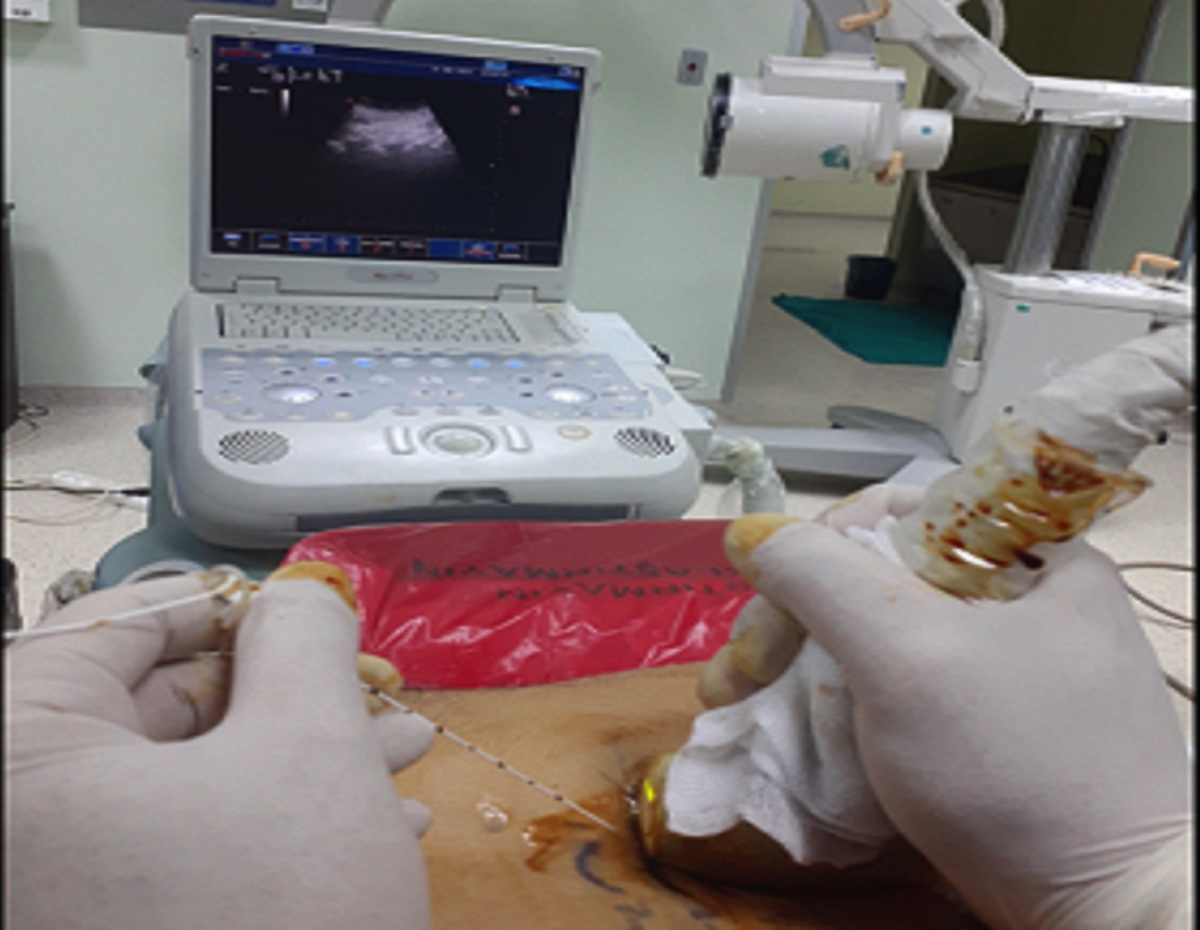 Figure 1 (B): The sagittal plane convex probe and needle orientation.
Figure 1 (B): The sagittal plane convex probe and needle orientation.
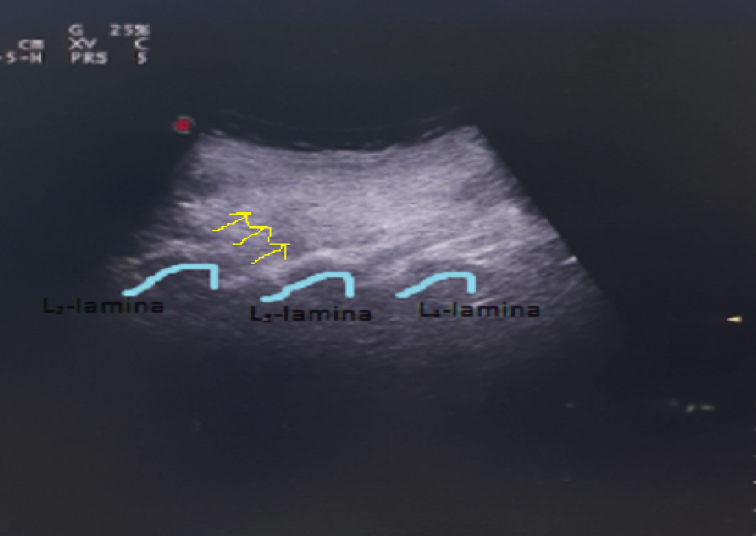 Figure 1 (C): The ultrasonographic visualisation of the needle and the lamina.
Figure 1 (C): The ultrasonographic visualisation of the needle and the lamina.
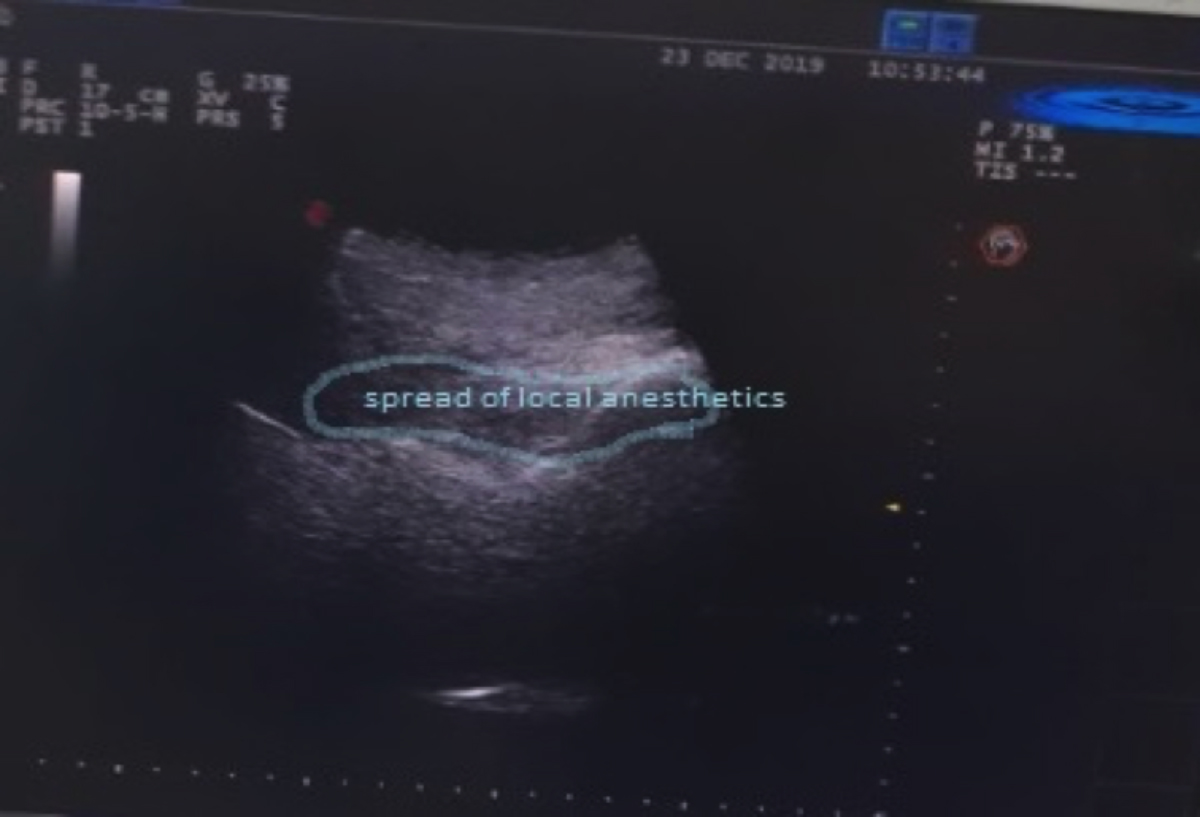 Figure 1 (D): The dispersion of local anesthetic over the lamina.
Figure 1 (D): The dispersion of local anesthetic over the lamina.
RLB has been in use for pain management of various conditions such as breast surgery, rib fracture pain, and lumbar trauma with or without using ultrasound guidance.3 In this case, the local anesthetic was injected into the deep paraspinal area between the vertebral lamina and the muscles above the lamina for obtaining postoperative analgesia. In RLB, the injection point is located closer to the midline and is more profound. Using this technique with ultrasound-guidance, reduces the possible risks of blind technique epidural injection.3
The injected local anesthetic has a limited craniocaudal distribution with the RLB technique, which may be due to the location of the injection point, the thicker muscle layer, and the tight attachment of muscle structures to the lamina.4 Therefore, RLB may lead to a better somatic and visceral analgesia in vertebral surgeries due to the distribution pattern on neural foramina and in epidural space.
In this report, we aimed to demonstrate the efficacy of RLB in pain management as a part of a multimodal approach for acute pain management of vertebral surgery. However, randomised clinical studies are required to explore our clinical observation.
CONFLICT OF INTEREST:
There is no any conflict of interest.
AUTHOR'S CONTRIBUTION:
KP: The author made the draft, design, editing, and review processes of the manuscipt.
REFERENCES
- Voscopoulos C, Palaniappan D, Zeballos J, Ko H, Janfaza D, Kamen V. The ultrasound-guided retrolaminar block. Can J Anesth 2013; 60(9):888-95. doi: 10.1007/s12630-013- 9983-x.
- Onishi E, Toda N, Kameyama Y, Yamauchi M. Comparison of clinical efficacy and anatomical investigation between Retrolaminar Block and Erector Spinae Plane Block. BioMed Research International 2019; 9:1-8. doi: 10.1155/2019/ 2578396.
- Adhikary SD, Bernard S, Lopez H, Chin KJ. Erector Spinae Plane Block Versus Retrolaminar Block: A Magnetic Resonance Imaging and Anatomical Study. Reg Anes Pain Med 2018; 43(7):756-62. doi: 10.1097/AAP.00000000 00000798.
- Murouchi T, Yamakage M. Retrolaminar block: Analgesic efficacy and safety evaluation. J Anesth 2016; 30(6): 1003-7. doi: 10.1007/s00540-016-2230-1.