Pakistan’s Health System Against COVID-19: Where Do Things Stand?
By Meesha Iqbal1, Aysha Zahidie2Affiliations
doi: 10.29271/jcpsp.2020.06.3ABSTRACT
The national response of Pakistan’s health system to COVID-19 was assessed by applying a framework of three distinct tiers. The first tier assessed politico-economic ecosystems: lockdown procedures, contact-screening, monetary/organisational arrangements for economically deprived groups, and travel restrictions. The second tier assessed intervention measures according to six building blocks of WHO: strategic vision highlighted by National Action Plan COVID-19, inadequacy and urban bias of healthcare professionals, expanded bed capacity, enhanced laboratory diagnostic capacity and financial assistance. The third tier of community participation revealed that the majority of the population was abiding by restrictions, but sporadic instances of orthodox religious gatherings were facilitating community spread. We recommend private health sector coordination with public facilities and call for deployment of non-practising health professionals. The neighborhood-warden-system should be introduced at the union council level with the help of community level volunteers to facilitate enforcement of quarantines and responding to emerging community needs.
Key Words: COVID-19, Coronavirus disease 2019, Pakistan healthcare delivery.
INTRODUCTION
The year 2020 will be remembered for its ghastly start, with COVID-19 hitting more than 200 countries in less than three months.1 The pandemic originated in Wuhan city in China, with the first suspected case dating back to November 17, 2019; by the end of January 2020, more than 7,000 people were affected.2,3Appropriate and timely measures by the Chinese government led to a flattening of the epidemic curve by the end of February 2020; simultaneously, the cases outside China began to rise globally.4 The World Health Organization (WHO) declared the outbreak a public health emergency of international concern on January 30 and a pandemic on March 11, 2020.5 As of June 15, 2020; 8,118,671 people had been affected globally, with 439,198 deaths (a 5.4% case fatality rate).1 The epicenter of COVID-19 has shifted from China to Spain, Italy, and the United States of America (USA); the USA now reports the highest absolute number of cases in the world (2,182,950 as of June 15).1
Pakistan, the fifth most populous country in the world with over 200 million people, shares its northern border with China.6 The first case of COVID-19 in Pakistan was reported on February 26, 2020. As of June 15; 148,921 confirmed cases of COVID-19 (675 cases per million of the population) and 2,839 deaths have been reported in the country.1
The health sector of Pakistan has traditionally suffered from “Mixed health systems syndrome,” with the public and private streams running parallel and less than 1% of gross domestic product (GDP) spent on health in national budgets (WHO benchmark: at least 6% of GDP).7,8 After the devolution of power in 2010, health has constitutionally been a provincial subject, such that the provinces have the mandate and responsibility for health planning, service delivery, financing, and human resource management.9 Pakistan faces the triple burden of disease along with frequent natural disasters such as earthquakes, heat waves, and floods. The National Disaster Management Authority (NDMA) is the top policy-making body for disaster mitigation and control in Pakistan.10 Although contingency plans for combating catastrophes exist, Pakistan does not have a coordinated national public health emergency plan for health-related emergencies.11 The country has a global health security index score of 35.5/100 and falls in the category of countries “least prepared” for epidemics and pandemics (country ranking: 105/195).12
A lack of coordination and role clarity between the federal and provincial governments, fragile health systems, scarce resources, and poor implementation at the district level, along with “demand” side issues of illiteracy and high population density, characterise Pakistan’s landscape. Amidst these challenges, it was sought to evaluate the national response of the health system of Pakistan to the COVID-19 pandemic according to scientific parameters.
FRAMEWORK OF ANALYSIS:
A framework was formulated by adapting and modifying the Kielmann’s health system framework and the six building blocks of the WHO to assess the national response of Pakistan to COVID-19 (Figure 1).13,14 The framework was organised into three tiers. The first tier related to the broader policy environment, the laws and guidelines formulated by the federal and provincial governments, and the economic, social, cultural, and political ecosystem for combating the virus. In the second tier, the capacity and performance of the health system of Pakistan was determined according to the six building blocks of the WHO. In the third tier, community participation and people’s attitudes, perceptions, and practices in the ongoing war against this invisible enemy, were assessed.
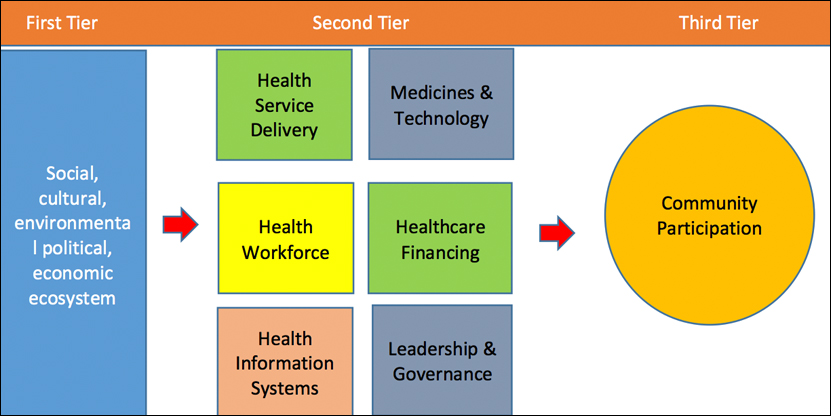 Figure 1: Analytical framework to assess the national health system’s response to COVID-19 in Pakistan.
Figure 1: Analytical framework to assess the national health system’s response to COVID-19 in Pakistan.
THE FIRST TIER:
The laws, guidelines, and strategies adopted by Pakistan were assessed in light of its political, economic, environmental, and socio-cultural ecosystem to combat COVID-19.
Transport restrictions and passenger screening:
The Government of Pakistan was proactive in initiating the pre-screening of passengers arriving from the Beijing airport more than a month before the index case unfolded in the country. Screenings were initiated simultaneously at four major airports for passengers coming from China on January 23, 2020.15 On January 30, flight operations between Pakistan and China were suspended and the land border was sealed, leaving 1300 Pakistani students stranded in China. The reopening of the Sino-Pakistan land border at Khunjerab Top, scheduled for February, was also postponed until April 2020.16
The Government was less swift to close the border with Iran, which had become the new epicenter at this time. Pilgrims crossing the Pakistan–Iran border at Taftan were allowed to enter Pakistan after being screened and quarantined.17 Many believe that this was a watershed moment, allowing COVID-19 to enter Pakistan as a result of inadequate infrastructure, inadequately trained staff, and ineffective quarantine measures at the Taftan isolation centre.18 Pakistan closed the border with Iran on February 23.19
Lockdown procedures:
Pakistan followed China’s aggressive and effective strategy of lockdown against COVID-19 to a moderate extent, within the country’s capacity to sustain the lockdown. All educational institutions were closed on March 13, 2020; this was followed by the gradual closure of shopping malls, industries, and transport systems.20,21 Only grocery shops, pharmacies, and hospitals remained open; the government and the military establishment were shown to be united on all fronts to make the lockdown operational.20
Pakistan is a developing country with 29% of the population (55 million) living below the poverty line and an estimated 3 million people working as daily wagers.22,23 Complete and sudden lockdown without a sustainability contingency plan was not deemed suitable in view of the country’s widespread poverty. The government announced a relief package of 200 billion rupees, amounting to 17,500 rupees per person for daily wage earners; subsidies for petrol, diesel, electricity, and gas; and standardized prices of essential food items in utility stores.24 The “Prime Minister’s Corona Relief Fund” was established to accumulate donations for those at risk of impoverishment by the lockdown,25 and a “Corona Relief Tiger Force,” comprising more than 3 million young people, was formed by the government to distribute food to the poor and create awareness about COVID-19 in areas under lockdown.26
Contact tracing:
The federal health minister stated that contact tracing for COVID-19 was started after only two confirmed cases in the country.27 The country’s intelligence agencies were tasked with mapping and cordoning off high-risk zones and ensuring the quarantine of diagnosed cases in many urban and rural areas. Unofficial reports claim that up to 20,000 contacts of COVID-19 positive cases have been mapped and are now being tested for the virus.
THE SECOND TIER:
The performance of the health systems of Pakistan was assessed across the six building blocks of the WHO.14
Health service delivery:
The hospitals of Pakistan have not yet been overwhelmed with confirmed cases of COVID-19; the total toll of laboratory-confirmed cases remains under 6,000 (as of April 12, 2020). There are 19,670 beds in the intensive care unit (ICUs) in Pakistan and 3,844 ventilators.28 The government was proactive in creating isolation centers, isolating and treating confirmed patients of the coronavirus in a safe and secure environment. The expo centers of the two biggest cities, Karachi and Lahore, were converted to 1,200 and 1,000 bed isolation centers, respectively.29,30 Pakistan Railways also converted 220 coaches with a total capacity of 2,000 hospital beds for COVID-19 patients.31 The capacity of quarantine facilities has been enhanced from 500 beds to 162,000. The government has also booked 1,795 three- and four-star hotels in which 40,000 patients can be accommodated if required.28
Another appropriate mitigation measure taken by the government was the establishment of a telemedicine web portal and corona mobile application, now providing free online consultation services to patients.32 The Young Doctors Association (YDA) also offered services to 150 doctors at its web portal.33 The private sector was also active in providing telehealth services.34 However, the preparedness efforts were focused on the urban population, with field hospitals established in metropolitan cities. Telemedicine is expected to help a limited number of the population because only 20% have internet access.35 Nonetheless, considering the limited options and meager resources of the country, the steps taken are encouraging.
Health workforce:
Pakistan has faced a shortage of doctors, nurses, and allied staff (doctor–population ratio: 1:1300; nurse–patient ratio: 1:50; nurses/ midwives per 1,000 population: 0.66), along with an imbalance in distribution, with a scarcity of health professionals in rural areas. There are 194,000 registered medical practitioners in Pakistan, of which 30,000 work in ICUs.28 Conditions have not yet been put under further strain during the COVID-19 pandemic. The country has focused its efforts on the prevention and control of the new coronavirus. The number of health professionals in public- and private-sector hospitals is still sufficient to deal with the incoming cases of COVID-19. They are also involved in the reverse tracing of household contacts of positive cases. However, it is anticipated that a severe shortage of health professionals could arise in the country with an increasing number of COVID-19 patients; because there is no pragmatic plan to respond. The National Institute of Health (NIH) in Islamabad has begun a series of training sessions for health professionals and clinical laboratories on infection prevention and control.36 The Sindh Healthcare Commission along with Medical Microbiology and Infectious Diseases Society of Pakistan (MMIDSP) has been conducting regular online sessions for healthcare professionals on infection prevention and control practices and correct use of PPE. So far, more than 700 healthcare professionals have benefitted from these sessions in the country.
Access to essential medicines and technology:
COVID-19 presents the double challenge of protecting healthcare workers and the patients. In China, of the 80,000 cases, more than 3,000 were healthcare workers (almost 4 %).37 Pakistan was initially faced with a lack of personal protective equipment (PPE) for health professionals, which was partially overcome by many donations from China, including but not limited to 500,000 surgical masks, 50,000 N95 respirators, 50,000 coronavirus testing kits, and 15,000 protective suits (as of April 1, 2020).28 Healthcare professionals in Pakistan have basic PPE (masks and gloves), which is also available at pharmacies for the public. Special protective gear for 30,000 health professionals working in ICUs is also available.38 There are nearly 2,200 ventilators available in public hospitals, and the number is expected to rise as a result of foreign donations by 1,000 and 3,000 by April 10 and 25, respectively.28
Fourteen laboratories are operating to detect COVID-19 in Pakistan, and the relevant authorities have been given access to data from private laboratories (as of April 3, 2020).38 Pakistan’s testing capacity has been enhanced from 30,000 to 280,000, and 61,801 tests had been performed by April 12, 2020.1,38,39 The laboratories have auto RNA extractors that make the test results available within 6 hours; however, only manual RNA extraction is available at mobile laboratories, which require at least 10 hours for the results.
Health information systems:
All the data pertaining to COVID-19 in Pakistan flow from district to provincial to federal level, where the data are assimilated by the NIH. In some districts, the WHO staff also provide support in terms of data management.39 Hospital, laboratory, screening, and quarantine data (that is, suspected cases in hospitals; those discharged, admitted and expired; total tests performed and total tests positive; travelers screened at the points of entry and number of suspected cases; and number of people quarantined at home or in facilities) are typically presented in the form of “daily situation reports” with provincial breakdowns. However, there could be gross underreporting of data because the private health sector is only marginally represented in the information provided, and not all the districts are reporting, particularly in rural areas.
Health systems financing:
With its limited healthcare budget, Pakistan is doing everything it can to tackle the menace of COVID-19. Sindh province released 7.21 billion rupees to combat COVID-19, of which 6.9 billion rupees were given to the Sindh health department to procure medicines, equipment, generators, food, sanitizers, testing kits, etc.40 The federal government released an 1.2 trillion rupees ( roughly $7 billion) in an economic plan to minimize the economic damage to vulnerable segments of society.41 There has been a massive number of donations to the Prime Minister’s Corona Relief Fund, and the country has received assistance from the World Bank in the form of $200 million in financial aid.28 However, the country still struggles to make the two ends meet.
Leadership and governance:
The presence of qualified health ministries at the federal and provincial levels, led by a resolute prime minister, has been a blessing for Pakistan as it sails through COVID-19.42 The Ministry of National Health Services, Regulation, and Coordination prepared the National Action Plan for COVID-19 Pakistan, outlining the strategic vision required by the health sector to control the disease.43 Advice on mitigation strategies was formed by the government, and mitigation measures were defined and demarcated.44 The standard operating procedures (SOP) for contact tracing, specimen collection, laboratory standards, case management, quarantine facilities, hospital waste management, waste management at the airports, and burial guidelines for COVID-19 were also elaborated to guide the health sector.45 Furthermore, there are plans to upgrade the laboratory capacity from 14 to 50, to adopt community screening in addition to contact screening, and to build field hospitals in consultation with Chinese experts. There is constant friction between provincial and federal governments in terms of lockdown procedures and financial packages, but the overall policy direction seems to be agreed between provinces and federal governments.
THE THIRD TIER:
As social distancing remains the mainstay in preventing the spread of COVID-19, community participation is fundamental to tackling the disease. Pakistan is under lockdown with variations in stringency across the provinces. Although 70% of the population is illiterate, the law enforcement agencies have ensured that the public abides by physical distancing policies. Big gatherings are non-existent, traffic is sporadic, and citizens are spread out in grocery and utility stores, wearing masks, or covering their faces with cloth. Even though the majority of the population is adhering to the restrictions, some religious factions, especially the “Tabligee Jamaat,” have disregarded the policy, holding a three-day gathering of 250,000 people in Raiwind (March 10–12, 2020).46 The event was blamed for an inordinate increase in the number of cases when 154 worshipers tested positive for COVID-19.46 On April 2, the entire city of Raiwind was placed under strict absolute quarantine, while more than 10,000 attendees were quarantined in 36 districts of the Punjab and Sindh provinces. Congregational prayers have been limited to five people in mosques, but time and again individuals have been reported barging in.
Huge support from the public has been seen, with more than 30,000 volunteers registering for the voluntary force declared by the Federal Government in just two days and vast amounts of money pouring in for the “PM Relief Fund” to aid daily wagers, people who had lost their jobs, and those made destitute by the lockdown.
CONCLUSION
Pakistan with its meagre resources has been trying to curb the worsening situation of Covid-19. The fragile health systems of Pakistan have been improved with increased bed capacity, diagnostic ability and enhanced provision of PPEs. The people of the country, with few exceptions have been compliant with the lock-down procedures. However, the situation might change for the worse as the cases multiply and pandemic unfolds in the country. We recommend certain measures to improve the landscape of response to Covid-19 in Pakistan (Box 1).
 Box 1: Recommendations to combat COVID-19 in Pakistan.
Box 1: Recommendations to combat COVID-19 in Pakistan.
CONFLICT OF INTEREST:
Authors declared no conflict of interest.
AUTHORS' CONTRIBUTION:
MI: Designed the study and prepared the first draft of the manuscript.
AZ: Provided technical assistance throughout the study.
All authors reviewed and approved the final draft of the manuscript.
REFERENCES
- Worldometers. (2020) [Internet]. Coronavirus cases. Retrieved from https://www.worldometers.info/coronavirus/.
- J Bryner. 1st known case of coronavirus traced back to November in China. Live Science [Internet]. Newyork. Retrieved from https://www.livescience.com/ first-case-corona virus-found.html
- Steven Jiang. China reports over 7,000 cases of Wuhan coronavirus cases. CNN. Beijing. Last updated January 29, 2020. Retrieved from https://www.cnn.com/asia/ live-news/coronavirus-outbreak-01-29-20-intl-hnk/index.html.
- Worldometers (2020). Coronavirus cases: growth factor of daily new cases. Retrieved from https://www. worldo meters.info/coronavirus/coronavirus-cases/#cases-growth-factor.
- WHO. Rolling updates on coronavirus disease (COVID-19) updated 9 April 2020. Retrieved from https://www.who.int/ emergencies/diseases/novel-coronavirus-2019/events-as-they-happen.
- World Population Review. Pakistan Population 2020. Retrieved from https://worldpopulationreview.com/ countries/pakistan-population/.
- Jowett M, Brunal MP, Flores G, Cylus J. Spending targets for health: no magic number. Geneva: World Health Organization; 2016 (WHO/HIS/HGF/HFWorkingPaper/16.1; Health Financing Working Paper No. 1); http:// apps. who.int/iris/bitstream/10665/250048/1/WHO-HIS-HGFHFWorkingPaper-16.1-eng.pdf.
- S Nishtar. Chapter 2, Health Systems in Pakistan. Choked pipes: Reforming Pakistan's Mixed. Health System 2010; 60(4).
- Constitution (Eighteenth Amendment) Act, 2010. The constitution of Pakistan. Retrieved from http://www. pakistani.org/pakistan/constitution/amendments/18amendment.html.
- National Disaster Management Authority. Islamabad. 2019,. Retrieved from http://www.ndma.gov.pk/aboutUs.php
- Shehla Zaidi. Withstanding health shocks. Dawn. 13 April, 2020 Retrieved from https://www.dawn.com/news/1544319.
- Global Health Security Index. 2019. John Hopkins Bloomberg School of Public Health. Centre of Health Security. Retreived from https://www.ghsindex.org/wp-content/uploads/2019/10/2019-Global-Health-Security-Index.pdf.
- District Health Planning Manual, toolkit for district health managers. Ministry of Health. Governement of Pakistan. Feb 2002.
- The world health report- health systems: improving performance. 2000. WHO.
- Dawn. Pakistan exercises caution as more cases of China's coronavirus surface in other countries. Updated 23 Jan 2020. Retrieved from https://www.dawn.com/news/1530103.
- Islamuddin Sajid.AA. Pakistan delays border opening with China. 31 Jan 2020. Retreived from https://www. aa.com.tr/en/asia-pacific/pakistan-delays-border-opening-with-china/1719702.
- Kaswar Klasra. This week in Asia. Pakistan quarantines hundreds of pilgrims from Iran, as it steps up efforts to contain coronavirus. 4 Mar 2020. Retrieved from https://www.scmp.com/week-asia/health-environment/article/3065053/pakistan-quarantines-hundreds-pilgrims-iran-it-steps.
- The News International. 12 Apr 2020. Who brought coronavirus to Pakistan from Iran? Retrieved from https://www.thenews.com.pk/print/633183-who-brought-coronavirus-to-pakistan-from-iran.
- Turkey and Pakistan close borders with Iran over coronavirus deaths. 23 Feb 2020. Retrieved from https://www. theguardian.com/world/2020/feb/23/turkey-and-pakistan-close-borders-with-iran-over-coronavirus-deaths.
- Aamir Latif and Islamuddin Sajid.13 Mar 2020. Pakistan closes schools, universities over coronavirus. Retrieved from https://www.aa.com.tr/en/asia-pacific/pakistan-closes-schools-universities-over-coronavirus/1765276.
- Tara Donaldson. Pakistan Lockdown Idles Factories—Where Orders Had Shriveled Up. 26 Mar 2020. Retrieved from https://sourcingjournal.com/topics/sourcing/pakistan-coronavirus-lockdown-garment-factories-closed-synergies-worldwide-levis-202444/.
- Arab News. Pakistan. Daily wagers say government’s virus relief package won’t cover minimum needs. 31 March 2020. Retrieved from https://www.arabnews.pk/node/ 1650116/pakistan.
- National Assembly Secretariat (34th Session) p. 18. Retrieved from http://www.na.gov.pk/uploads/ documents/questions/1470057800_189.pdf.
- The News International. PM Imran allocates Rs200bn relief package for daily-wagers amid coronavirus outbreak. 12 Apr 2020. Retrieved from https://www.thenews.com.pk/latest/ 633880-pm-imran-allocates-rs200bn-relief-package-for-daily-wagers-amid-coronavirus-outbreak.
- Geo News. PM Imran sets up coronavirus relief fund, urges Pakistanis to donate. 01 Apr 2020. Retrieved from https://www.geo.tv/latest/280327-pm-imran-sets-up-coronavirus-relief-fund-urges-people-to-donate.
- The News International. Over 300,000 apply for Corona Relief Tiger Force. 12 Mar 2020. Retrieved from https:// www.thenews.com.pk/print/638759-over-300-000-apply-for-corona-relief-tiger-force.
- Twitter. Zafar Mirza @zfrmrza. Mar 2020. https://twitter. com/zfrmrza?lang=en.
- Sana Jamal. World Asia. Pakistan. 27 Mar 2020. China sends tonnes of medical aid to Pakistan to fight COVID-19. Retrieved from https://gulfnews.com/world/asia/pakistan/ china-sends-tonnes-of-medical-aid-to-pakistan-to-fight-covid-19-1.70663601.
- Faizan Ali Warraich. 24 Digital. First phase of 1,000-bed field hospital at Lahore’s Expo Centre completed. 24 Mar 2020. Retreived from https://www.24newshd.tv/24-Mar-2020/ first-phase-of-1-000-bed-field-hospital-at-lahore-s-expo-centre-completed.
- The News International. Coronavirus: Pakistan Army helps set up field hospital at Karachi's Expo Centre. 13 Apr 2020. https://www.thenews.com.pk/latest/631969-coronavirus-pakistan-army-helps-set-up-field-hospital-at-karachis-expo-centre.
- VOA News. Pakistan Railway Converts Train Cars Into COVID-19 Isolation Units. 31 Mar 2020. Retreived from https://www.voanews.com/science-health/coronavirus-outbreak/pakistan-railway-converts-train-cars-covid-19-isolation-units.
- Daily Times. 13 Apr 2020. Pakistan. In a first, governor inaugurates Corona Telemedicine Web Portal. Retreived from https://dailytimes.com.pk/578965/in-a-first-governor-inaugurates-corona-telemedicine-web-portal/.
- The Express Tribune. Corona telemedicine portal, App introduced. 19 March 2020. Retrieved from https:// tribune.com.pk/story/2179012/8-corona-telemedicine-portal-app-introduced/.
- Telehealth for coronavirus (COVID-19). Liaquat National Hospital. Retreived from https://www.lnh.edu.pk/Pages/ teleHealth.
- National Institute of Population Studies (NIPS) [Pakistan] and ICF. 2019. Pakistan Demographic and Health Survey 2017-18. Islamabad, Pakistan, and Rockville, Maryland, USA: NIPS and ICF.
- National Institute of Health. Islamic Republic of Pakistan. Past events. Retreived from https://www.nih.org.pk/ past-events/.
- Jared Kaltwasser. Coronavirus: For Healthcare Workers, Risk of Infection, But Also Burnout. 15 Mar 2020. https:// www.contagionlive.com/news/for-health-care-workers-risk-of-infection-but-also-burnout.
- Sana Jamal. World Asia. COVID-19: Pakistan rapidly setting up new labs, buying ventilators, testing kits. 31 Mar 2020. https://gulfnews.com/world/asia/pakistan/covid-19-pakistan-rapidly-setting-up-new-labs-buying-ventilators-testing-kits-1.70729066.
- Ministry of National Health Services, Regulations and Coordination. Daily Situation Report –PakistanCOVID-19April 03, 2020 https://www.nih.org.pk/wp-content/uploads/ 2020/04/COVID-19-Daily-Updated-SitRep-03-April-2020.pdf.
- Hafeez Tunio. The Express Tribune. Karachi's Expo to become 10,000-bed isolation center, 19 Mar 2020. https://tribune.com.pk/story/2179314/1-karachis-expo-become-10000-bed-isolation-center/.
- Uzair Younus. Atlantic Council. Coronavirus hits Pakistan’s already-strained economy, and its most vulnerable. 30 Mar 2020. https://www.atlanticcouncil.org/blogs/new-atlanticist/ coronavirus-hits-pakistans-already-strained-economy-and-its-most-vulnerable/.
- S Siddiqi. Tackling the challenge of Covid-19 in Pakistan: expecting wonders from a fragile helath system. Dawn. 6 Apr 2020. https://www.dawn.com/news/1546850/tackling-the-challenge-of-covid-19-in-pakistan-expecting-wonders-from-a-fragile-health-system.
- National action plan for corona virus disease (COVID-19) Pakistan. Government of Pakistan. Ministry of National Health Services, Regulations and Coordination. https:// app.adpc.net/sites/default/files/public/publications/attachments/National%20Actional%20Plan_compressed.pdf.
- Advisory on mitigation startegies Covid-19. Governement of Pakistan. 11 Mar 2020. https://www.nih.org.pk/wp-content/ uploads/2020/03/Advisory-on-Mitigation-Stratgey-updated-12-March-2020.docx.pdf.
- 45. National Institute of Health. Islamic Republic of Pakistan. COVID-19. Retreived from https://www.nih.org.pk/novel- coranavirus-2019-ncov/.
- South China Morning Post. South Asia. Fears of massive Pakistan coronavirus outbreak after 100,000 attended Lahore religious gathering. 5 Apr 2020. Retrieved from https://www.scmp.com/news/asia/south-asia/article/3078479/fears-massive-pakistan-coronavirus-outbreak-after-100000.