An Archetypal Variant of Peripheral Adenomatoid Odontogenic Tumour
By Selma A, Sreela LS, Philips Mathew, Twinkle S. Prasad, Admaja K. NairAffiliations
doi: 10.29271/jcpsp.2021.03.361Sir,
A 12-year boy presented with the chief complaint of an asymptomatic slowly growing swelling on the attached gingiva of the labial surface of left maxillary central incisors for one year. On intra-oral examination, a well-defined solitary nodular swelling of 0.7×0.5 cm was noted on the attached gingiva of the labial surface of maxillary left lateral incisors, extending from the mesial aspect of the central incisor to the mesial aspect of the lateral incisor (Figure 1). On palpation, the swelling was non-tender, smooth surfaced, and of firm consistency. The case was provisionally diagnosed as fibrous epulis with differential diagnosis of other reactive lesions of the gingiva, such as peripheral ossifying fibroma. The intra-oral periapical radiograph revealed a bony erosion with respect to the inter-dental area between the central and lateral incisors, beginning at the level of middle-third, and extending upto the apical-third of radicular portion of lateral incisor. Subsequently, an excisional biopsy was performed and specimen was sent for histopathological examination. The histopathology revealed fibrous capsule with proliferating spindle and cuboidal cells arranged in duct-like structures and rosettes. The scattered duct-like structures showed lumen of varying sizes, and were lined by single layer of cuboidal to columnar epithelial cells with nuclei polarised away from the lumen. Stellate reticulum-like spindle cells were seen between the duct- like structures (Figure 2). The stroma was loose with irregular to round calcified bodies seen in- between. A diagnosis of peripheral adenomatoid odontogenic tumour (PAOT) was made.
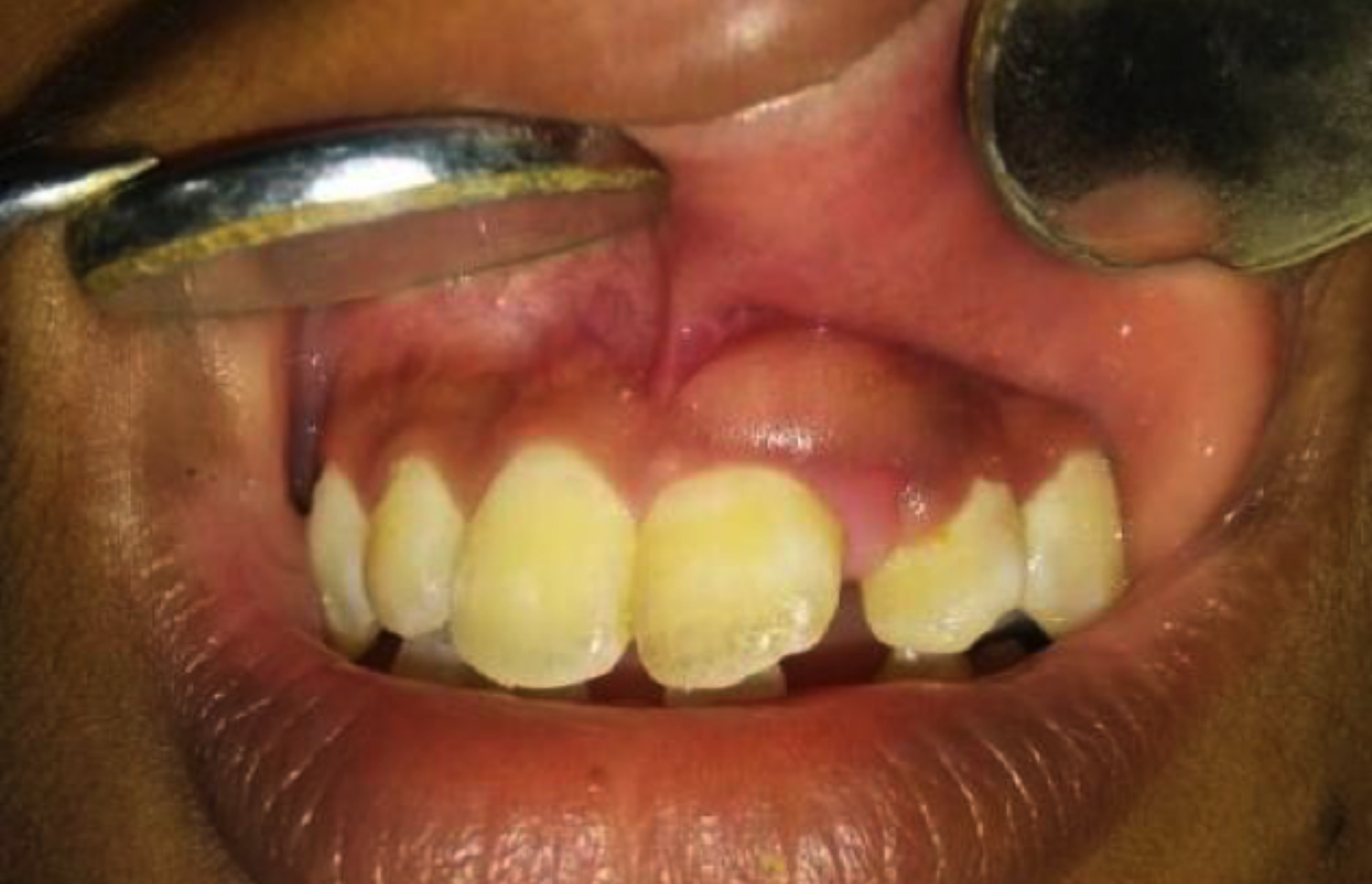 Figure 1: Solitary well-defined swelling on the attached gingiva.
Figure 1: Solitary well-defined swelling on the attached gingiva.
PAOT is one of the rarest odontogenic tumours constituting only about 3% of all odontogenic tumours.1 The rarity of the lesion and its ambiguous presentation makes it a diagnostically challenging entity. The clinical presentation mimicking reactive lesions of the gingiva along with minimal bony changes in the radiograph can easily misguide the diagnosis. PAOT usually manifests in younger age group with a female predilection, favouring maxillary anterior region. 2 The radiographic evaluation will not yield any striking bony changes and the histopathology is the ultimate diagnostic part that reveals true microscopic nature of the lesion.3
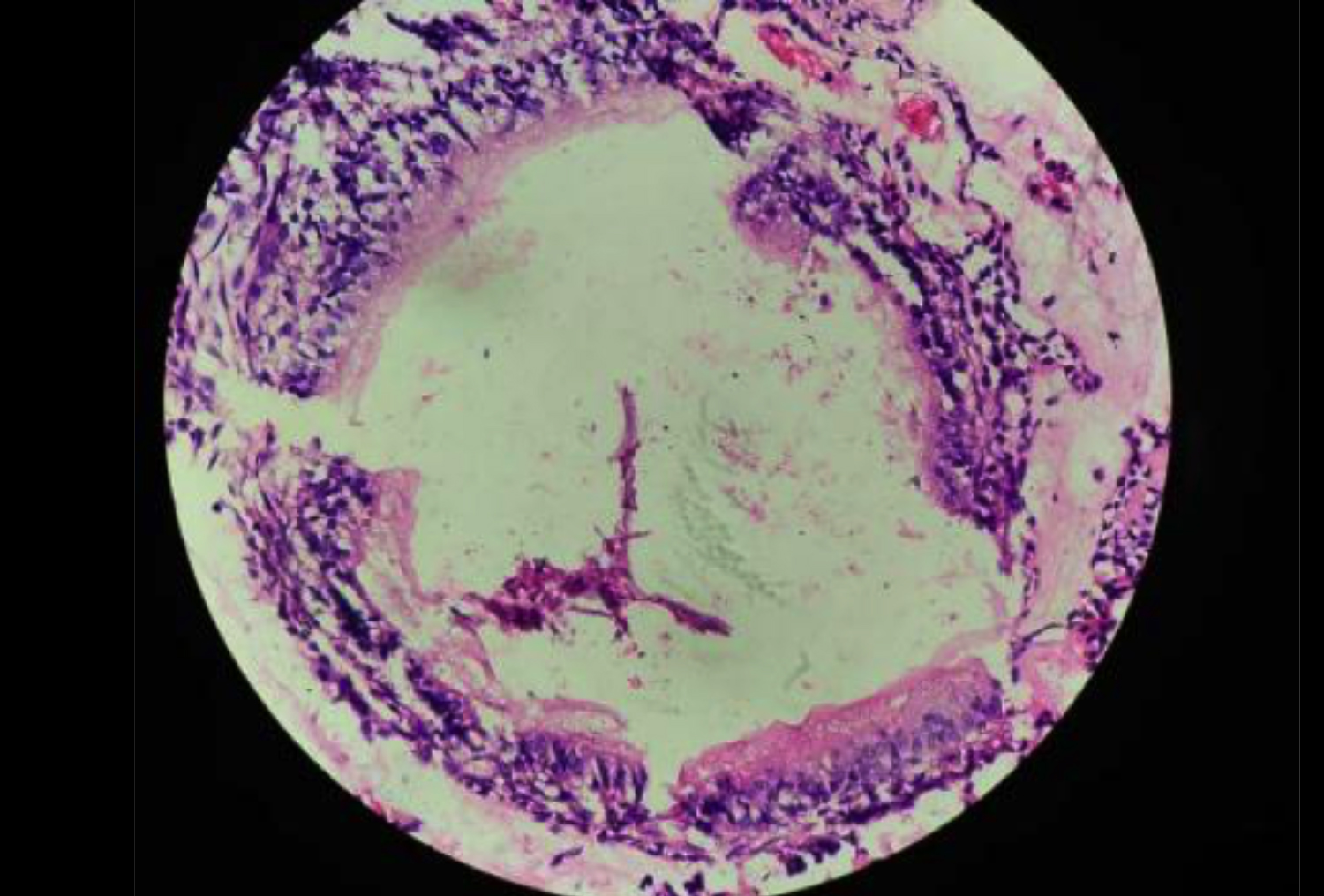 Figure 2: High-power view of one of the duct-like structures, lined by cuboidal to columnar cells with polarised nuclei. Stellate reticulum like spindle cells are seen between the duct-like structures. (H&E, ×200).
Figure 2: High-power view of one of the duct-like structures, lined by cuboidal to columnar cells with polarised nuclei. Stellate reticulum like spindle cells are seen between the duct-like structures. (H&E, ×200).
Due to its clinical resemblance, PAOT can easily be mistaken for innocent reactive lesions of the gingiva, so it is recommended to go for histological evaluation for the ultimate diagnosis. Conservative surgical excision with adequate margins is the treatment modality, which was done in the present case; and overall prognosis is excellent. The recurrent cases were only two till date.4
CONFLICT OF INTEREST:
The authors declared no conflict of interest.
AUTHORS’ CONTRIBUTION:
SA, PM: Connectional design of the work, analysis and interpretation of the data. Agreement to be accountable for all aspects of work.
TSP: Drafting the work and revised it.
SLS, AKN: Final approval of the version.
REFERENCES
- Jindwani K, Paharia YK, Kushwah AP. Surgical management of peripheral variant of adenomatoid odontogenic tumor: A rare case report with review. Contemp Clin Dent 2015; 6(1):128-30. doi: 10.4103/0976-237X.149309.
- Jain MK, Oswal KS. Adenomatoid odontogenic tumor of mandible-‘‘master of disguise”. J Dent App 2014; 1(3): 40-2.
- Prakash SMR, Vidisha G, Nagaraju K, Sangeeta M, Swati G. Peripheral adenomatoid odontogenic tumor: A rare case report. Annals Clin Case Reports - Oral Med 2017; 2:1-4.
- Dwivedi D, Prabhakar N, Kasetty S, Ahuja R. Peripheral adenomatoid odontogenic tumor in a cloak of an epulis: Report of a rare case. BMC Oral Health 2019; 19(1):81. doi: 10.1186/s12903-019-0759-8.